Table of Contents
What are food allergies and how do you prevent food allergies in your child? Understanding what food allergies are and how they affect the body is the first step in allergy prevention and management. There is a lot of buzz on the internet and social media about elimination diets and food sensitivities or intolerances; but true food allergy is a much more serious issue, and must be handled as such. With the help of a good pediatric food allergist who is accessible, empathetic, and knowledgeable, you can manage your child’s food allergies more efficiently.
What are Food Allergies?
A food allergy is an immune system response to something the body deems as dangerous. When an allergen is ingested, the immune system deploys a variety of components including antibodies (called immunoglobulins) and white blood cells that cause symptoms ranging from mild to severe. These symptoms as well as how they are managed, depend on which types of immune cells are involved.
Immunoglobulin E (IgE) plays a large role in the rapid onset of allergy symptoms; IgE circulating in the bloodstream can cause swelling and itching of the tongue and mouth, runny nose or watery eyes, increased heart rate, difficulty breathing, coughing, wheezing, vomiting, and even dizziness or confusion and this usually occurs within minutes of ingesting an allergen.
A mild IgE-mediated allergy that usually develops in later childhood or adulthood is known as Oral Allergy Syndrome (OAS). OAS is a rapid onset of an itchy/scratchy feeling in the mouth, or swelling of the lips, tongue, and throat. Some people experience itchy ears as well. This mild reaction does not typically extend beyond the tissues of the mouth and resolves quickly once the offending food is swallowed and no more of the food is ingested.
A more severe IgE response is anaphylaxis, which causes system-wide symptoms such as rapidly dropping blood pressure, increased heart rate, tongue or airway swelling, skin rash, shock, unconsciousness, and (if not addressed quickly) death. Anaphylaxis is a medical emergency and caregivers of children who experience anaphylactic reactions to food, need to be prepared to respond to this emergency at all times.
Sometimes other parts of the immune system are involved in allergic reactions. These types of reactions are usually a little slower to develop, most often within two-to-six hours rather than within minutes. White blood cells called eosinophils are a potential culprit and cause a local inflammatory reaction, usually to the throat, stomach, or intestines. Reactions from this type of immune response are usually more related to the gastrointestinal system and include symptoms like bloating, nausea, vomiting, and abdominal pain. Prolonged exposure to inflammatory markers can cause extreme swelling to the throat which causes difficulty swallowing or even choking.
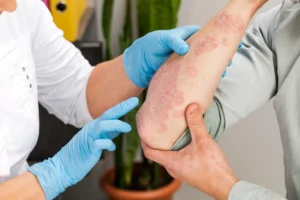
Inflammatory responses can also affect the skin and disrupt the natural barrier of the skin, leading to dry, cracked, red, and itchy or painful eczema rashes. These breaks in the skin also increase the risk of bacteria getting into the body and causing secondary infections.
When the immune system directly attacks the tissues of the body, chronic illness can result; Celiac Disease is an example of this. When gluten is ingested, non-IgE immune cells attack the lining of the intestines and damage it, leading to abdominal pain, diarrhea, fatty stools, and eventually, poor nutrient absorption and negative impacts on growth.
Who is Affected by Food Allergies?
Current CDC estimates indicate that 1 out of every 13 children (8% of children in the US) have a food allergy. Children under the age of five have a higher rate of allergies than their five-to-seventeen-year-old counterparts, and the rate of allergies are equal for boys and girls. Data also indicate that the rate of childhood food allergies is rising, with an over 18% increase from 1997 to 2007 and trending upwards in more recent years. The rate of hospitalizations related to food allergies has also increased. Healthcare providers are unsure if some of this has to do with increased awareness and more precise diagnostic methods, or if the rate of allergies is actually increasing.
Risk Factors for Allergies
There is also ongoing debate as to whether genetic or environmental factors play a greater role in the development of allergies than originally thought. Having a parent or sibling with food allergies increases a child’s risk of developing allergies themselves. Research indicates that children with healthy parents have a 5-15% chance of developing food allergies, but when one parent has an allergy, the risk increases to 40%. Children of two parents with allergies have a 60-80% risk! Children with other allergic disorders like asthma or atopic dermatitis (eczema) are also at an increased risk of having a food allergy. On the other hand, children with food allergies are two-to-four times more likely to be diagnosed with asthma or other allergic conditions like eczema.
Hygiene, lifestyle, and diet also play a role in the risk of having allergies. Higher levels of pollution, preservatives, artificial ingredients in food, and even milk-based infant formula, are linked to increased rates of food allergy.
Allergies and Gut Microbiome
Emerging evidence show that gut microbiome likely plays a role in the risk of developing food allergies A microbiome is a collection of microbes like bacteria, viruses, and fungi that naturally live in our bodies. The microbiome of children with allergies differs from those without allergies even before allergies develop. Imbalances in the gut microbial system precede the development of food allergies.
Environmental factors also shape gut microbiome in early life (particularly the first three months of life before foods are even ingested). Breastfeeding and virginal birth seem to reduce the risk of developing allergies. The protective effect of vaginal birth is due to the presence of microbes in the birth canal. Exposure to pets and being outdoors offers some protective qualities against allergies while the use of milk-based infant formula and high fat diets negatively impact the microbiome and potentially increases the risk of allergies.
It is important to note that some children, even with all these protective factors, may still develop allergies while those without access to any of these protective factors may be allergy-free. These are new and emerging facts so parents and caregivers should not worry about past choices they made or past experiences outside of their control. Instead, focus on creating a healthy and balanced environment moving forward to support your child’s overall well-being.
The purpose of these studies is simply to learn more and, in the process, adopt practices or interventions with the potential to reduce the risk of food allergy. Practices such as delayed bathing of newborns which has recently become widely recommended, is one recommended way to reduce the risk of allergies.
Common Allergens in Childhood
So what are the most common foods that cause allergies? Technically, anything can be an allergen if it triggers the immune system; however, according to the U.S. Food and Drug Administration, 90% of all food allergies are from one of nine foods:
- Milk
- Eggs
- Peanuts
- Tree nuts
- Fish
- Shellfish
- Soy
- Wheat
- Sesame (added Jan 1, 2023)
Depending on the allergen and the type of allergic response, sometimes cooking the food at high temperatures changes the protein enough that an allergic response does not occur; for example 70-80% of children with milk or egg allergies can eat baked goods containing eggs and milk without triggering a reaction.
Cow’s milk allergy is of particular concern for infants because standard infant formula is made with cow’s milk protein. This protein (along with soy) is also one of the few that can cross into breast milk, and so, even breastfed infants can have an allergic response to cow’s milk protein if their mother consumes enough in her diet. Gastrointestinal symptoms, fussiness, widespread eczema rash, and poor growth are all concerning signs of a cow’s milk allergy in infants. Switching to an amino-acid formula, or breastfeeding mothers eliminating dairy from their diet may be necessary. Thankfully, 50% of children with cow’s milk allergy outgrow it by their first year and 90% outgrow it by three years old.
Other childhood allergies may be outgrown as well, with 80% of children eventually outgrowing egg, milk, and wheat allergies. Nut and seafood allergies often last into adulthood and for life, with only 20% outgrowing those allergies in childhood.
Commonly confused for allergies
Lactose intolerance may commonly be miscategorized as an allergy, but this is actually an intolerance to dairy related to a person’s lack of an enzyme to digest it properly. Since the immune system is not involved in lactose intolerance, it is not considered an allergy. Celiac Disease is an immune-mediated response to wheat, and so is an allergy; however, some people may experience symptoms when consuming gluten (bloating, gas, abdominal pain, vomiting, and diarrhea) without any immune system involvement. This group of symptoms is considered a gluten intolerance rather than an allergy.
Preventing Food Allergies
As recently as 15 years ago, common advice to prevent childhood food allergies was to delay exposure to common allergens until their third year, depending on the food. However, this recommendation was simply based on expert opinion and had no evidence to back it up. In recent years, extensive studies into childhood food allergies have actually revealed the opposite to be true; early exposure to potential allergens, especially for children at high risk, may actually be protective against the development of allergies.
As the evidence grew to support this theory, recommendations around allergy prevention began to change. In 2008, the American Academy of Pediatrics (AAP) changed its recommendation to suggest that while solids should still be delayed until four-to-six months of age, exposure to potential allergens did not need to be delayed beyond this. In 2015, the AAP took this a step further to recommend food with a high-allergen risk should be introduced as early as possible to potentially decrease the risk of developing an allergy. This has been shown to be especially true for children at high risk of developing an allergy, such as those with asthma, eczema, or a first degree relative with a food allergy.
There are several ways to introduce high-allergen risk foods to your child, but the appropriateness of solid foods and risk of choking should still be taken into account. Solid foods should not be offered to babies less than four months old, with six months or older being ideal. Signs of readiness include being able to sit up and support the head independently and being able to grab objects using a raking motion or pincer grasp. Baby-led weaning is a popular method of introducing solid foods where purees are not used, and instead, food is offered in soft, small pieces for babies to play with and try eating at their discretion. After your child has tried and done well with pieces of some fruits and vegetables and seems able to move on to other foods, you can begin to incorporating potential allergic foods.
Small pieces of cooked eggs, wheat containing breads like muffins or pancakes, or well-cooked fish can be offered as children explore different tastes and textures. Nut butters are thick and may be difficult for infants to chew and swallow, but peanut powder is an easy-to-use method of introducing nuts and can be mixed into pureed foods or sprinkled over pieces of solid food. Whenever any new food is introduced, babies should be watched closely for any sort of rash, coughing, choking, or other reaction. It is also recommended to allow three-to-four days in between each new food before trying another one. This allows for easy identification of the food causing an issue if a reaction does occur.
In addition to early exposure to a variety of foods, additional things parents can do to try and prevent food allergies is to focus on a varied and nutritious diet during pregnancy and breastfeeding once the baby arrives.
Living With Allergies
For about 4-6% of children, allergies will still occur despite appropriate efforts to prevent them. For these children, how this is managed depends on the type of food and the severity of the reaction. For all allergies, avoiding the food is necessary to prevent symptoms; even small amounts can be enough for the immune system to take action within seconds.
From an early age, children should be taught about their allergies and reminded to ask if an allergen is present in foods before accepting them from others. Making teachers and coaches aware of allergies and having an Allergy Action Plan (FARE’s Food Allergy & Anaphylaxis Action Plan) on hand should be routine.
If a child has an extreme reaction, particularly anaphylaxis or any airway involvement, being prepared for accidental exposures and emergencies is paramount. Even if they are never used, having un-expired, easily accessible EpiPens on hand is extremely important. Parents, and children when they are old enough, should be trained annually on how to use an EpiPen and the EpiPen should be in a known location at home, in a child’s backpack if appropriate, a parent’s bag, and other locations outside of the home.
A treatment option known as immunotherapy exists in different forms although many of them are still in the early stages of development. Immunotherapy works by repeatedly exposing the body to small amounts of an allergen, building the dose over time, to desensitize the body and raise the dosage needed for a child to experience a reaction. Immunotherapy does not offer a cure for food allergies but may provide peace of mind and improve quality of life for children and families living with food allergies so a child is able to have an accidental exposure to an allergen without a life-threatening response. There is, however, one FDA-approved, standardized method of oral immunotherapy for peanut allergy, PALFORZIA, which is a precisely-dosed capsule containing peanut protein available for children ages four and older with a peanut allergy.
For less extreme or more chronic reactions, other treatments may be useful, such as steroid inhalers where the medicine is swallowed instead of inhaled. This helps reduce inflammation along the digestive tract. For symptoms affecting the skin, a careful regimen of unscented soaps and skin-barrier-protecting moisturizers, as well as steroid creams for flare ups, is usually employed. As previously mentioned, special formula may be needed for infants or elimination diets for breastfeeding mothers.
Any time an elimination diet is needed, especially if multiple foods are restricted, a child’s growth and development should be followed closely so that nutritional deficits do not develop. Supplementation with various vitamins or minerals a child may be lacking may be needed. An example would be providing a child with a milk allergy with calcium and vitamin D supplements. Partnering with the best food allergist near you as well as a qualified dietitian can be a useful option to ensure children do not become malnourished.
Experts are still researching and expanding existing knowledge on what exactly causes food allergies and how we can prevent them. Currently, there are some promising leads, but overall, we just have a good grasp on risk factors, many of which are not easily changed, and so, sometimes, little can be done to prevent true food allergies from occurring. Luckily, many children outgrow their food allergies and the possible methods of treatment are growing. If you are concerned about your child developing food allergies, talk to your child’s pediatric allergist about their potential risk factors and what to watch for as you introduce foods to your child.